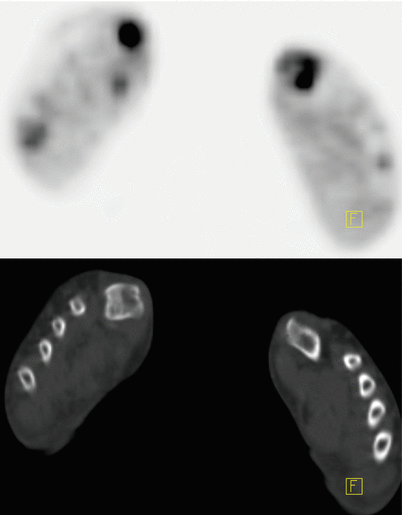
A focal (nodular) form of FCC may appear as a mass with spiculated or smooth margins ( Figures 7-4 and 7-5 ). It may appear as prominent nonmasslike enhancement in regional, focal, or segmental distribution ( Figures 7-2 and 7-3 ). FCC has a wide spectrum of morphologic and kinetic features on MRI. The risk of developing carcinoma is increased to 1.5 to 2 times when FCC is associated with moderate or florid ductal hyperplasia and increased 5 times with the presence of atypia.įCCs do not have specific mammographic or sonographic findings other than cyst formation. There is no increased risk for the subsequent development of breast carcinoma in women with non-proliferative FCC. It is common in younger women, affecting one third of females 20 to 45 years of age. The histologic findings include cyst formation, apocrine metaplasia, mild epithelial hyperplasia, stromal fibrosis, and mild adenosis. B, Postcontrast subtraction image is needed to confirm the absence of contrast enhancement within the dilated ducts.įibrocystic change (FCC) refers to a constellation of benign breast changes that represent normal but exaggerated, hormonally mediated breast tissue response. A, T1-weighted fat-suppressed noncontrast image shows dilated retroareolar ducts containing high signal intensity proteinaceous fluid. Focal enhancement within the duct lumen would raise concern for intraductal papilloma or carcinoma.ĭuct ectasia is seen in a 61-year-old breast and ovarian cancer susceptibility ( BRCA) gene–positive woman undergoing high-risk screening MRI. Because of such signal hyperintensity on precontrast images, postcontrast subtraction images are usually needed to confirm absence of contrast enhancement ( Figure 7.1, B ).

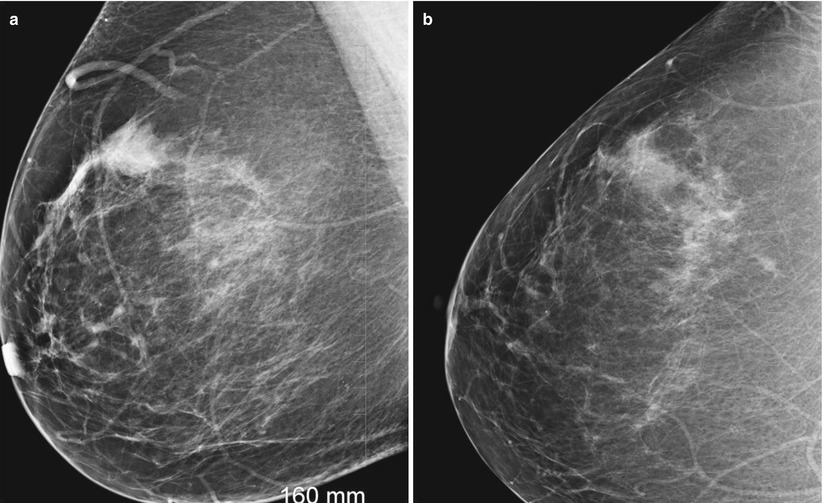
More often, the fluid is hyperintense in signal on T1-weighted images because of proteinaceous or hemorrhagic contents ( Figure 7.1, A ). The contents of the ducts may show signal intensities similar to that of water, hypointense on T1-weighted images and hyperintense on T2-weighted sequences. They appear as non-enhancing, fluid-filled, often branching, tubular structures converging toward the nipple. On MRI, ectatic ducts are usually incidental findings. Mammographically, the calcified proteinaceous secretions within dilated ducts appear as bilateral symmetric rodlike “secretory calcifications.” Ultrasonography will demonstrate dilated ducts filled with anechoic fluid, without or with debris. Some may present with spontaneous and intermittent clear to yellow nipple discharge. Others suggest that duct dilation is the primary event, caused by obstruction of the ducts leading to secondary inflammation owing to leakage of duct contents. Some consider all inflammatory processes as the initiating event, leading to destruction of the elastic network of the duct with subsequent duct ectasia and periductal fibrosis. It has been found in women of all ages, and its etiology is unknown.
This chapter describes the MRI appearances of common and uncommon benign findings.ĭuct ectasia is a nonspecific dilation of the major subareolar ducts, with occasional involvement of smaller ducts.
Some benign lesions, however, are simply indistinguishable from malignancy on imaging, and biopsy is necessary for histologic diagnosis. It is important for radiologists to be familiar with these benign findings because it will enable them to select lesions for biopsy with improved specificity and to better assess radiologic-pathologic concordance of biopsy results. Even with careful selection of patients, radiologists usually encounter benign findings more frequently than malignant lesions when interpreting breast MRI. The current practice of breast imaging calls for using breast magnetic resonance imaging (MRI) only on high-risk patients with appropriate indications to maximize cancer detection yield and minimize the false-positive rate.
